Jordan Rau reports for Kaiser Health News that for quite some time nursing homes have not been following basic protocols to contain the spread of viruses and bacteria. The situation has only gotten worse since 2017. And, because assisted living facilities are not subject to government health inspection, we have no clue how well they do in containing the spread of viruses and bacteria.
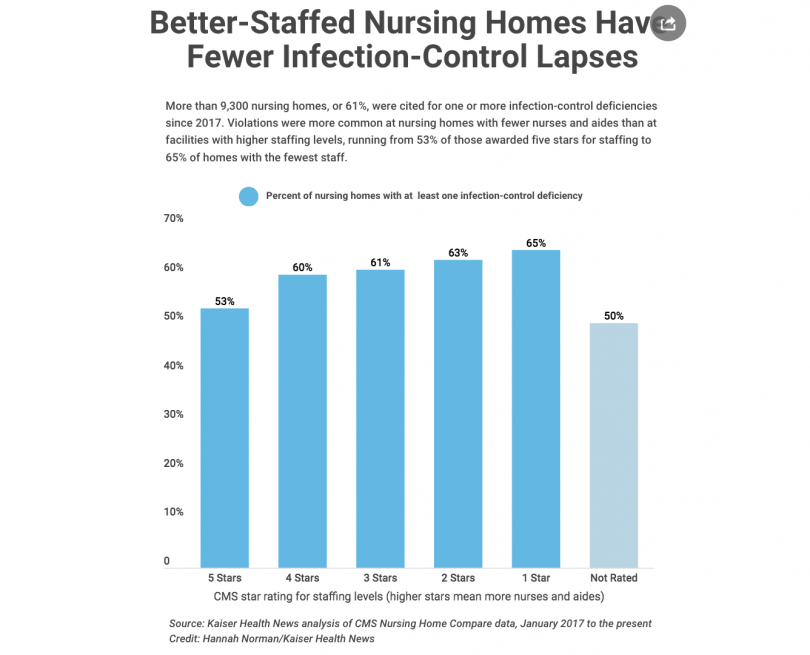
Kaiser Health News found that more than six in ten nursing homes–9,372 nursing homes–have received citations from government inspectors for deficiencies in controlling infections. Those nursing homes with fewer staff had a greater likelihood of receiving a citation. It’s another reason to avoid chain nursing homes, which tend to have fewer staff.
When choosing a nursing home, bear in mind that the government’s star-rating system tells you very little about the quality of a nursing home. Forty percent of five-star nursing homes have been cited for infection-control deficiencies. Five people at Life Care Center of Kirkland, Washington, which has a five-star rating, have died of the coronavirus.
Facilities that have been cited for deficiencies often have workers who do not wash their hands each time they see a patient or do not wear masks or gloves when they are with contagious patients. These deficiencies can cause infections to spread.
Health inspectors treat these deficiencies as minor in almost all instances, so nursing-facilities have no incentive to change their practices. Only in 109 out of 13,000 citations were these deficiencies treated as serious threats to patients. Nursing homes with these deficiencies are generally not fined or penalized in terms of their star ratings. But, between the flu and MRSA or other antibiotic resistant bacteria, each year nursing homes have as many as 3.8 million infections which kill about 388,000 residents.
In some instances, staff who are sick do not stay home and infect other staff and nursing home residents. And, when staff stay home, it can sometimes be difficult for nursing homes to find replacement staff. There is a shortage of health care workers across the US.
As of 2016, the Centers for Medicare and Medicaid Services requires an infection preventionist–an employee in charge of infection control–to undertake training and work part-time or full-time in every nursing home. But, the Trump administration has proposed to do away with this on-site staff person. It wants the preventionist simply to spend “sufficient time” at a nursing home to oversee infection-control initiatives, whatever that means.
Here’s more from Just Care: