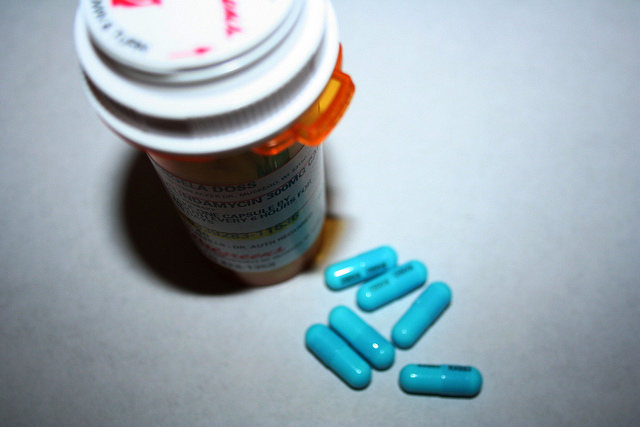
It’s bad enough that lack of competition empowers drug companies to set prices sky high for so many important drugs. And, not surprisingly, one in four people in the U.S. say that they struggle to pay for the drugs they need. It turns out that, if you have drug coverage, your drug copay may be higher than the drug’s cash price, and your pharmacist won’t tell you.
Bloomberg news reports that pharmacy benefit managers PBMs, which contract with pharmacies to pay for drugs on behalf of your health plan, force pharmacists to charge you the insurer’s copay, even when the pharmacy sells the drug for less. These PBMs or at least Optum Rx and Catamaran, owned by UnitedHealth Group and Humana’s subsidiary PBM, forbid pharmacists from telling you that you’ll save money if you don’t use your insurance to get the drug.
How does the deal between the PBM and the pharmacy work exactly? The pharmacy turns over the difference between the copay and the actual cost to the PBM. And, according to KARE11, the PBM shares in the profits with the health plan.
For example, KARE11 found at pharmacy:
- Doxycycline copay: $46.14 v. cash price $26.95.
- Venlafaxine copay: $67.13 v. cash price: $24.99
The extent to which the health plan benefits from these PBM “clawback” contracts is not clear. But, we’re talking real money. Because of these deals between PBMs and pharmacists, consumers are handing over hundreds of millions of dollars to the PBMs. Not surprisingly, there are more than a dozen lawsuits against insurers contracting with PBMs that are leading people to pay more for their drugs than they should.
If you are struggling to pay for your drugs, you might consider buying your drugs online or abroad, as millions of Americans are now doing.
And, if you want Congress to rein in drug prices, please sign this petition.
Here’s more from Just Care:









Another good reason to get for-profit insurance companies out of our health care and institute a single-payer system!
It is no wonder that our medical costs are twice as great as the next highly industrialized countries’. This type of kickback should be, and probably is already, illegal. How about sending a few of these PBMs and pharma executives to jail under the RICO statutes?
The Connecticut legislature passed a bipartisan bill to stop this gag on pharmacists. The following interview discusses the Democrat Governor’s pro- industry hostility to the law. Both Repubs and corporate Dems are bad on many health issues, serving their donors instead of the common good. When Dems Help Big Pharma (w/ David Sirota) – YouTube
https://m.youtube.com/watch?v=yEQS6mCJqFg
went to pharmacy to pick up my wife’s prescription which had been 20/month and suddenly it was 450.00 so I asked the pharmacist to use my veterans discount card instead of using the “Scamthem” insurance plan and suddenly it was 63.00 clearly showing kickbacks are now OK, these insurance companies operate just like the mafia back in the day and should be returned to non profit only business models under heavy scrutiny as well as stopping big pharma and medical device companies from paying off doctors behind closed doors which used to be illegal due to conflict of interest.